You’ve heard of pseudoscience — but what about celebrity science?
New research suggests a bombshell claim from Mel Gibson on influencer Joe Rogan’s popular podcast may have helped fuel a dramatic surge in prescriptions for an unproven cancer treatment.
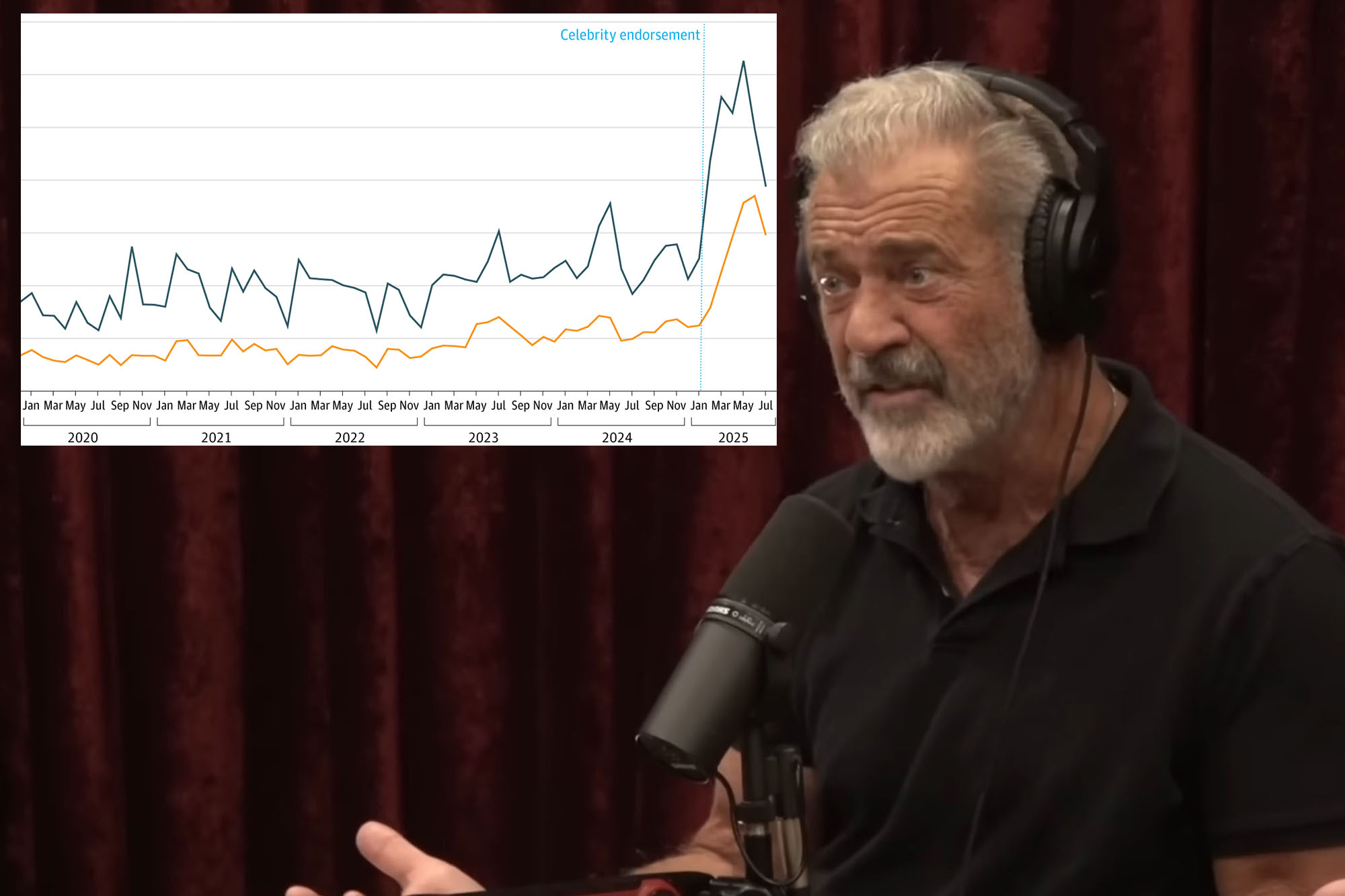
During the January 2025 episode, which racked up more than 60 million views in its first month, the actor-director claimed three friends with Stage 4 cancer were cured after taking the off-label regimen.
The controversial drugs at the center of the frenzy were ivermectin — an antiparasitic that became a flashpoint during the Covid-19 pandemic — and fenbendazole, a veterinary dewormer that isn’t FDA approved for humans. Gibson claimed all three of his friends no longer had the disease “at all” after taking the medications.
In the months after his remarks, prescriptions for the combination jumped, with the steepest increases among young men, white patients and those in the South. Among cancer patients, prescription rates were more than 2.5 times higher, while in the South they surged to more than three times their 2024 levels.
But experts caution there is little clinical evidence to support the drugs for this use.
In laboratory cell and animal studies, ivermectin and fenbendazole have shown some anti-cancer activity — but the doses required for even a modest effect would typically be considered toxic in humans, according to Dr. Skyler B. Johnson of the University of Utah Huntsman Cancer Institute.
Johnson, who was not involved in the study, told CIDRAP News he is also concerned ivermectin could interfere with how the body processes cancer treatments and other medications.
To date, no human clinical trials have shown that ivermectin and fenbendazole are safe or effective for treating cancer.
The study’s authors sounded the alarm that following unproven advice could cost them their lives.
“As a primary care doctor, I want my patients and people across the country to have the chance to get treatments we know can help them live longer, healthier lives,” Dr. John N. Mafi, senior author of the UCLA-led study, said in a press release.
“When prescribing for an unproven cancer treatment more than doubles after a single podcast, especially among men and people in the South, it raises a concern that patients may be skipping or delaying treatments we know work in favor of something that hasn’t been proven to help them,” he warned.
Co-author Dr. Katherine Kahn, a professor of medicine at UCLA, stressed that “not all widely shared health information is accurate, even when it comes from familiar or influential sources.”
“Using unproven treatments can carry real risks, especially if it delays care that is known to work,” she said.
The researchers stressed that the study does not prove the podcast directly caused the spike in prescriptions.
It also remains unclear whether patients were taking the drugs alongside standard cancer treatments — or instead of therapies such as chemotherapy or radiation.
But the findings add to growing concerns among doctors over ivermectin’s off-label use.
The drug became a lightning rod during the Covid-19 pandemic after being promoted on social media by influencers, politicians and even some physicians as a treatment and preventive measure.
Now ivermectin is once again back in the headlines, with some online claims suggesting it could help treat hantavirus following a deadly outbreak aboard a luxury cruise ship.
Experts say there is still no high-quality evidence in humans showing ivermectin works against either Covid-19 or hantavirus.
And while the National Cancer Institute announced earlier this year that it is studying ivermectin’s possible anti-cancer properties, the research remains in the preclinical stage — meaning any findings are still far from being ready for actual patients.
The UCLA-led study raises major questions that researchers say should be explored in the future, including whether patients are replacing proven cancer therapies with the drug combo, whether the treatments are causing harm and which doctors are prescribing them.
“We often focus on how to efficiently get evidence into practice,” said study lead author Dr. Michelle Rockwell of Virginia Tech.
“But these findings remind us that some forces can influence care very quickly. The challenge for health systems is how to meet patients in that moment with information that is both timely and trustworthy.”